
What Can You Do at Every Meal to Reduce Your Risk of Heart Disease?
You may be thinking, “Well, this is an easy question. Simply reduce or eliminate the amount of saturated and hydrogenated fats, refined sugars, and total calories you consume at a meal,” and you would be right, and we should all work to achieve these healthy nutritional guidelines.
However, regardless of how hard we try we often fall short of eating according to recommended guidelines on a consistent basis. Fortunately, there is a very positive and impactful intervention that we can all make at mealtime that has shown to provide significant protection against the major pathological mechanisms of atherosclerosis that can lead to cardiovascular disease (CVD) or heart disease.
What Happens When We Eat a Meal?
First, there are several processes that take place when we consume food – digestive, endocrine, neurological, etc. to name a few, and all are important and even contribute to the enjoyment of the meal.
However, there are a number of physiological responses that take place in the body during the hours following consumption of a meal (called the Postprandial Period or Postprandial Response) that have the potential to cause harm to our bodies.
These include damage to endothelial cells that line the walls of our arteries, hyperactivity of our blood platelets, oxidation of LDL cholesterol in our blood and an increase in inflammation in the cardiovascular system.
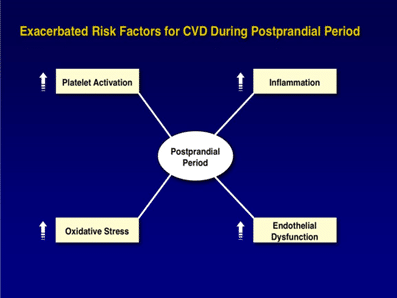
All of these risk factors or pathological mechanism responses that become elevated during the hours following a meal contribute to atherosclerosis or the progressive narrowing and hardening of our arteries due to the buildup of plaque.

Let’s look at each one of these pathological mechanisms separately to see how they individually and collectively contribute to the process of atherosclerosis.
Damage to the Endothelial Cells of Our Arterial Walls
Lining the inner surface of our arteries is a single layer of endothelial cells. These cells play a very important role in maintaining the integrity and functionality of our vessels.
Specifically, healthy endothelial cells release nitric oxide (NO) that functions to repel blood platelets, white blood cells and other debris from sticking to the wall of the artery, and when released in sufficient amounts cause the vessel to dilate for enhanced blood flow.
If these endothelial cells were to become damaged and rendered dysfunctional, the buildup of these cells and other debris overtime, in conjunction with oxidized cholesterol, forms the plaque that builds up in the walls of our arteries.
Endothelial cells can be damaged by a number of lifestyle habits and risk factors including cigarette smoke, high blood sugar (diabetes), high blood pressure (hypertension), and high blood cholesterol levels (hypercholesterolemia).
Specific to the focus of this article, a meal that is high in total caloric content, refined sugars, and saturated and/or hydrogenated fats has been shown to cause damage to endothelial cells during the postprandial period.
Blood Platelet Hyperactivity
A healthy, normal level of blood platelet activity is essential to helping us control bleeding in our bodies. They also play a vital role in helping heal damaged endothelial cells by releasing what is called platelet derived growth factors (PDGF) that promote the healing of damaged endothelial cells.
This is very important and as we previously mentioned there are some lifestyle habits and risk factors that damage these cells.
Unfortunately, the same risk factors that can damage endothelial cells also cause platelets to become hyperactive. As part of our body’s healing process, hyperactive platelets are drawn to the site of damaged endothelial cells (to aid in their healing) in excessive numbers (hyperactivity), and subsequently release excessive amounts of platelet derived growth factors (PDGF).
The PDGF work to heal the damaged endothelial cells, but because it has been released in excessive amounts, it diffuses through the inner lining of the arteries and stimulates the vascular smooth muscular cells (VSMC) of the middle arterial layer, causing them to divide and multiply aggressively.
Consequently, this excessive division and multiplication of the VSMC causes them to migrate inward into the opening of the artery, effectively narrowing the opening and negatively affecting blood flow through the vessel.
Inflammatory Response to LDL Cholesterol Oxidation
Our bodies are constantly subjected to free radicals (oxidants). Free radicals form as a natural byproduct of our own metabolism, can be found in certain foods or beverages we consume, are present in polluted air we may breathe, etc. These oxidants are unstable oxygen molecules and can “oxidize” and effectively alter LDL cholesterol molecules and damage body tissues.
Fortunately, we have antioxidants in our body that can neutralize the free radicals. Some of our antioxidants are endogenous or manufactured by our bodies, and others we must consume in our diet. If we maintain a good balance between the number of free radicals and antioxidants, our cells are not damaged, and LDL cholesterol is not oxidized.
However, if our LDL cholesterol becomes oxidized, our body’s immune system perceives the oxidized (changed/altered) LDL cholesterol molecule as a foreign intruder to the body’s well-being. Through complex chemical reactions our body’s immune system is activated to combat this foreign threat. In response, white blood cells (WBC) circulating in the blood are drawn to the site of the oxidized LDL cholesterol.
As these WBC’s pass through the inner layer of our arteries, they are converted to macrophages (MAC)and begin scavenging the oxidized LDL cholesterol molecules, similar to what they would do to invading pathogens (bacteria, viruses, etc.).
When they become engorged with the oxidized LDL cholesterol the MAC’s are then referred to as foam cells. These foam cells accumulate in the arterial walls and contribute to the development of atherosclerotic plaque.
Overtime, this plaque buildup causes narrowing of the artery leading to the development of cardiovascular disease. This process can occur over years and decades as the plague gradually accumulates before the problem leads to a heart attack, or a stroke if occurring in the arteries that feed the brain.
What Can We do to Combat these Pathological Mechanisms that Occur During the Postprandial Period?
Because these physiological responses that occur during the few hours after consumption of our meal – a time in which our cardiovascular system is under significant attack by these pathological mechanisms – we need an intervention with each meal that will reduce or negate these pathological responses and provide protection against heart disease.
The answer to the key question posed in the title of this article is to be sure and consume polyphenolic compounds (flavonoids) with each meal.
There are over 4,000 identified flavonoids and they are found in fruits, vegetables, nuts, seeds, and plant derived beverages like wine, tea, and fruit juices. They have extraordinary powerful properties including the ability to counteract the pathological mechanisms that are taking place during the postprandial period, as well as increase cardiovascular protection from a temporary increase in the protective HDL cholesterol and endothelial cell function.
This protection also includes a positive impact on blood pressure values as the vessels dilate more efficiency reducing the resistance to blood flow.
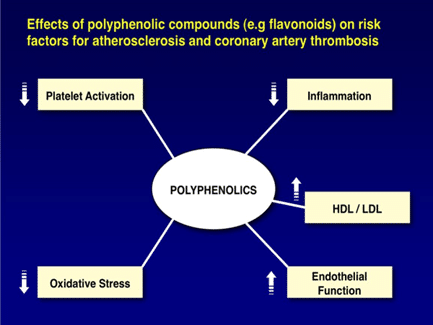
The targeted and timely (with a meal) consumption of these polyphenolic compounds/flavonoids can blunt the negative effects while providing healthy constituents to your diet.
Below are various ways to ensure that your meals, whether the nutritional content is good or not so good, include polyphenolic rich foods for a timely intervention against the pathological postprandial responses and their damage to our cardiovascular system.
For Breakfast
- Include a cup of berries with your cereal or whatever you eat in the morning. It really does not matter the kind of berry as all have various flavonoids that can offer some protection.
- Drink a 100% natural fruit juice such as purple grape juice, pomegranate, apple, orange or another berry juice. Research has shown that purple grape juice and pomegranate juices and red wine contain more of the types of flavonoids that promote cardiovascular health.
During Lunch
Lunch seems to be a time when a lot of folks eat out, whether that be at a fast-food restaurant or some quick grab-and-go food place. Unfortunately, the food options available at these types of places tend to be high in total calories, refined sugars, and saturated fats – all of which are associated with greater postprandial responses – and hence the need for a flavonoid rich component that you “add” to a typical lunch.
Consider bringing along your own fruit to help blunt the effects of the postprandial response. Again, the key is to always include a source of flavonoids whenever you consume significant calories, especially if those calories contain a lot of saturated fats or sugars.
If you are eating your lunch at a nice restaurant, whatever meal you select, be sure to include a fruit or vegetable with your order.
Evening Meal
The evening meal tends to be the time where many people consume a lot of calories. Drinking a glass of red wine or purple grape juice or pomegranate juice with your meal has shown to provide significant cardio protective benefits against the pathological mechanisms of the postprandial response.
A worthy goal is to always include a fruit and/or vegetable with your dinner.
Other Considerations
The consumption of alcohol in any form may be a risk for some individuals and therefore should be avoided. A person with diabetes may avoid drinks that are high in sugars, as are natural fruit juices as part of their efforts to control their blood sugar levels.
Overweight and obese individuals who are working hard to reduce caloric intake and improve body composition may choose to avoid foods and drinks that are high in caloric value during their weight loss efforts. And some simply do not like the taste of red wine, purple grape juice or pomegranate juices.
For these individuals, there are supplement products such as grape seed and grape skin extracts that may potentially offer benefits like those found in red wine and purple grape juice. As these substances are not regulated by the FDA, their potency and bioavailability may be questionable. However, some have been tested and offer benefits associated with blunting the postprandial responses.
It should also be noted that as a “supplement,” these products would be effective to help “supplement” your total dietary flavonoid intake. In doing so, keep in mind that several epidemiological studies have shown an inverse relationship between death from CVD and the total intake of flavonoids.
In conclusion, consuming a polyphenolic/flavonoid rich food/drink with each meal will help to reduce the negative pathological mechanisms occurring in our cardiovascular system during the hours following a meal. It is literally a timely and targeted intervention to protect your heart and vessels from disease.
Let’s Have a Conversation:
How will you incorporate these strategies into your meal planning to obtain protection against the post prandial pathological mechanisms that lead to heart disease?
Disclaimer: This article is not intended to provide medical advice. Please consult with your doctor to get specific medical advice for your situation.
Tags Healthy Eating







Very good article that goes deeper to explain the whole process.
I have berries most days & definitely a variety of veggies, fruit, eggs, fish, chicken & a bit of red meat occasionally. A treat occasionally, but the majority of the time its easy to eat from the ‘rainbow’ if i plan ahead.
Lunch for me was half slice of sourdough bread with tuna salad made with Genova Yellowfin Tuna in Olive Oil and some mayonnaise. A plate of mixed greens with black lentils. A blood orange on the side.
Be more direct. Tell people bluntly to cut down on saturated fats, meats, dairy, animal products. Vegans have very low rates if coronary heart disease, especially if they consume whole-food plant based diets.
as I’m reading this article I got a big smile on my face. I made myself some lunch and starting grazing. Opened my iPad to your a article and looked at my plate. Two rice cakes a this layer of almonds and sliced apples . I gave myself a big ataboy!!!